Guided bone regeneration (GBR) is a surgical procedure that utilizes bone grafts with barrier
membranes to reconstruct small defects around dental implants. This procedure is
commonly deployed on dehiscence or fenestration defects ≥2 mm, and mixing with
autogenous bone is recommended on larger defects.
Guided Bone Regeneration
Treatment
About This Treatment
The Process
Guided Bone Regeneration (GBR) is a surgical procedure that
uses barrier membranes and often bone grafts or other
biocompatible materials to encourage the body to regenerate
lost bone around a tooth or in an area where the tooth has been
extracted. This procedure is often utilized in conjunction with
dental implant placement when there is insufficient bone to
support the implant. Below is a simplified step-by-step guide to
a typical GBR procedure.
Comprehensive Evaluation
- Dental Examination:
- Detailed oral examination and health history review.
- Imaging:
- Utilizing X-rays and possibly 3D imaging (such as a CBCT scan) to assess bone quantity and quality.
- Treatment Plan Discussion:
- Exploring procedure steps, potential risks, benefits, alternatives, and answering any patient queries.
Pre-Surgical Phase
- Oral Hygiene:
- Ensuring optimal oral hygiene to prevent infection post-surgery.
- Health Consideration:
- Evaluating and managing any health conditions that may impact surgical outcomes.
The Surgical Procedure
- Anesthesia:
- Administering local anesthesia or sedation to ensure patient comfort during the procedure.
- Accessing the Bone:
- Creating a flap to access the bone defect area.
- Cleaning the Area:
- Removing any diseased or compromised tissue from the site.
- Bone Graft Placement:
- Placing bone graft material (which could be the patient’s bone, donor bone, or synthetic materials) in the area where bone regeneration is desired.
- Barrier Membrane Placement:
- Positioning a barrier membrane over the graft material to prevent fast-growing soft tissue from inhibiting bone growth.
- Suturing:
- Securing the area with sutures, ensuring the graft material and membrane are stable.
Recovery Period
- Healing Time:
- Allowing several months for the bone to regenerate in the grafted area. Healing times can vary depending on individual circumstances and the extent of the surgery.
- Post-Operative Instructions:
- Following detailed care and hygiene instructions, as well as dietary recommendations.
- Temporary Restoration:
- If relevant, utilizing a temporary restoration (such as a denture or bridge) to maintain aesthetics and function during the healing period.
Follow-Up and Monitoring
- Post-Operative Check:
- Ensuring proper healing, suture removal, and monitoring bone development through follow-up appointments.
- Secondary Procedures:
- If the GBR is a preparatory step for implant placement, planning the implant surgery after adequate healing and bone regeneration.
Final Restorative Procedures
- Implant Placement:
- If the GBR was performed to facilitate dental implant placement, the subsequent implant surgery will be planned once satisfactory bone regeneration is confirmed.
- Restoration Placement:
- Affixing the final restoration (such as a crown or bridge) onto the dental implant after it has integrated with the regenerated bone.
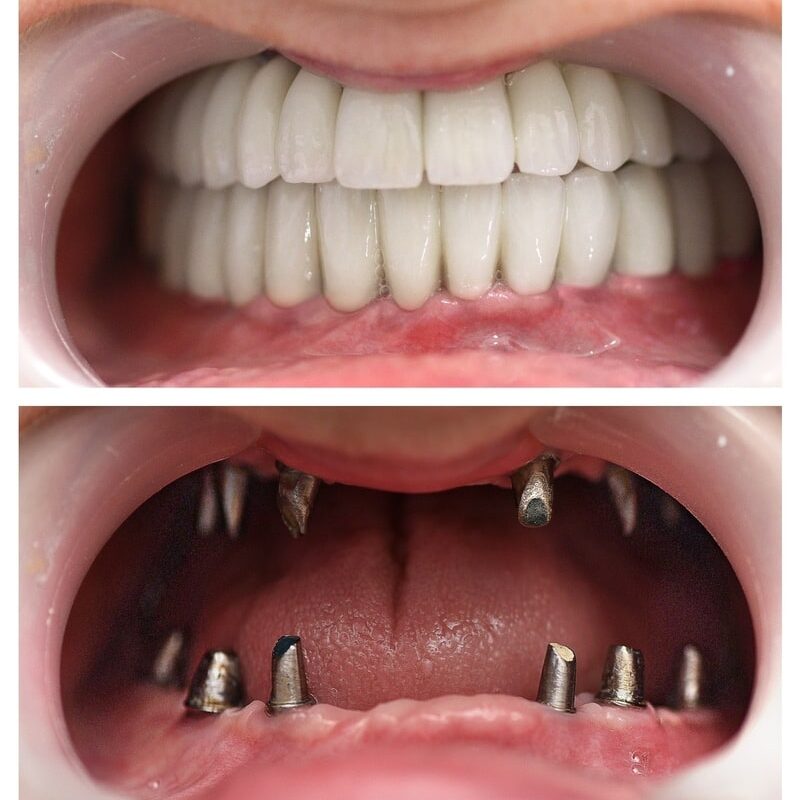
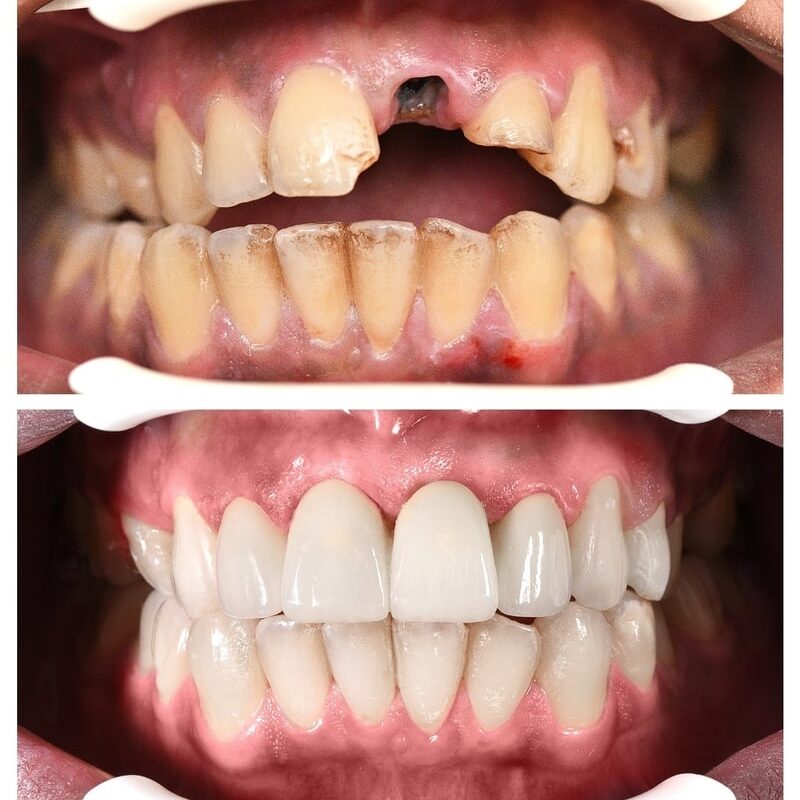
Before and After
SEE OUR RESULTS
Patient Stories
The Dental Implant Institute has been an excellent dentist surgery that I have been attending as a patient for many years. When I was young I didn’t have a pleasant experience with my local dentist on more than one occasion. I found the dentist at The Dental Implant Institute very reassuring and comforting. The management…
A great surgery; Dr Javier in particular spent time with me to make sure my new night guards fitted well and were up to the job
I lost my two front teeth whilst at school and had complications for years. Unfortunately I ended up needing an implant – which I had been avoiding! I wish I had done it sooner. Dr Javier was fantastic and guided me through each stage. He was always contactable to answer any queries or concerns. Very…
FAQs
Can you elucidate the scientific and clinical premise underlying Guided Bone Regeneration (GBR)?
Guided Bone Regeneration (GBR) operates on the principle of utilizing barrier membranes to orchestrate a defined space that favors the selective proliferation of osteogenic (bone-forming) cells. Scientifically, the technique relies on the biological concept of excluding non-osteogenic cell populations from the bony defect, thereby mitigating their inhibitory impact on bone regeneration. Clinically, GBR navigates through creating a stable and protected environment, often supplemented with bone graft materials, which acts as a scaffold for the new bone to develop, ensuring that the spatial and biological requisites for optimal bone regeneration are meticulously upheld, particularly in the context of implant dentistry.
How long does bone graft take to heal?
Recovery time depends on the injury or defect being treated and the size of the bone graft. Your recovery may take 2 weeks to 3 months. The bone graft itself will take up to 3 months or longer to heal. You may be told to avoid extreme exercise for up to 6 months.
Does bone graft turn to bone?
Bone grafting is possible because bone tissue has the ability to regenerate completely if provided the space into which it has to grow. As natural bone grows, it generally replaces the graft material completely, resulting in a fully integrated region of new bone.
What differentiates various materials and membranes employed within GBR and how are they selected?
The assortment of materials and membranes within the GBR paradigm emanates from various origins – autogenous, allogeneic, xenogeneic, and alloplastic – each with unique attributes and indications. Membranes, pivotal for GBR, can be resorbable or non-resorbable, with each offering distinct advantages and considerations. The selection of specific materials and membranes is sculpted by numerous factors, such as the defect’s size and configuration, the patient’s healing capacity, and potential anatomical and biological challenges. Clinical decision-making entwines scientific evidence with practitioner expertise to select materials that align with the clinical scenario and desired outcomes.
How does GBR intersect with dental implantology and what implications does it carry for implant placement and success?
GBR intricately intertwines with dental implantology by offering a methodology to augment deficient alveolar bone, thereby creating a robust foundation for implant placement. GBR can enhance the predictability of achieving optimal implant positioning, both functionally and aesthetically, by regenerating bone in regions of insufficiency. Consequently, it supports implant stability, facilitates biomechanical harmony, and can significantly impact the aesthetic outcomes, especially in visually pertinent zones, thereby weaving a crucial link between bone regeneration and the long-term success of dental implants.
What are the potential challenges and complications associated with GBR, and how can they be mitigated?
GBR, while potent, is not devoid of potential challenges and complications. These can encompass membrane exposure, infection, inadequate volume of regenerated bone, or undesirable healing outcomes. Meticulous surgical technique, stringent post-operative protocols, and adept management of the soft tissue are pivotal to mitigate potential complications. Precise case selection, comprehensive treatment planning, and realistic expectation management form the bedrock upon which successful GBR outcomes are sculpted, ensuring challenges are anticipated and adeptly navigated through the clinical journey.
Can GBR be universally employed across varied bone defect typologies and what determines its applicability?
The universality of GBR across varied bone defect typologies is inherently influenced by the defect’s characteristics, patient factors, and practitioner expertise. Certain defect morphologies, such as contained defects, traditionally respond favorably to GBR, while extensive or non-contained defects might necessitate adjunctive techniques or alternative regenerative strategies. Patient-related factors, such as systemic health, local factors, and compliance, also critically impact the applicability and success of GBR, thereby determining its viability within the specific clinical milieu.
How does the healing and post-operative trajectory following GBR unfold, and what does it imply for patient management and expectations?
The healing trajectory following GBR is characterized by a phase of initial clot stabilization, followed by cellular migration, proliferation, and gradual bone matrix deposition and maturation. Post-operative management encompasses meticulous adherence to protocols to safeguard the surgical site, including avoiding mechanical trauma, adhering to prescribed medications, and abiding by dietary recommendations. Patients must be apprised of the timelines, potential sensations, and any limitations that emerge during the healing phase, ensuring expectations are aligned with the clinical reality and healing biology.
In the context of future advancements and technological integrations, how might GBR evolve in its application and efficacy within regenerative dentistry?
The evolution of GBR within regenerative dentistry potentially looms on the horizon, embracing advancements in materials science, biotechnology, and digital integration. Future GBR applications might see the advent of more biologically active membranes and graft materials, potentially leveraging growth factors, gene therapy, or stem cell technologies to enhance regenerative capacities. Additionally, digital technologies might further streamline treatment planning, material customization, and surgical execution, thereby augmenting the precision, predictability, and overall efficacy of GBR in navigating through complex regenerative demands.
Book your consultation
Every journey begins with a detailed consultation. Our approach is always
bespoke, and your plan is individualised for you and your concerns.