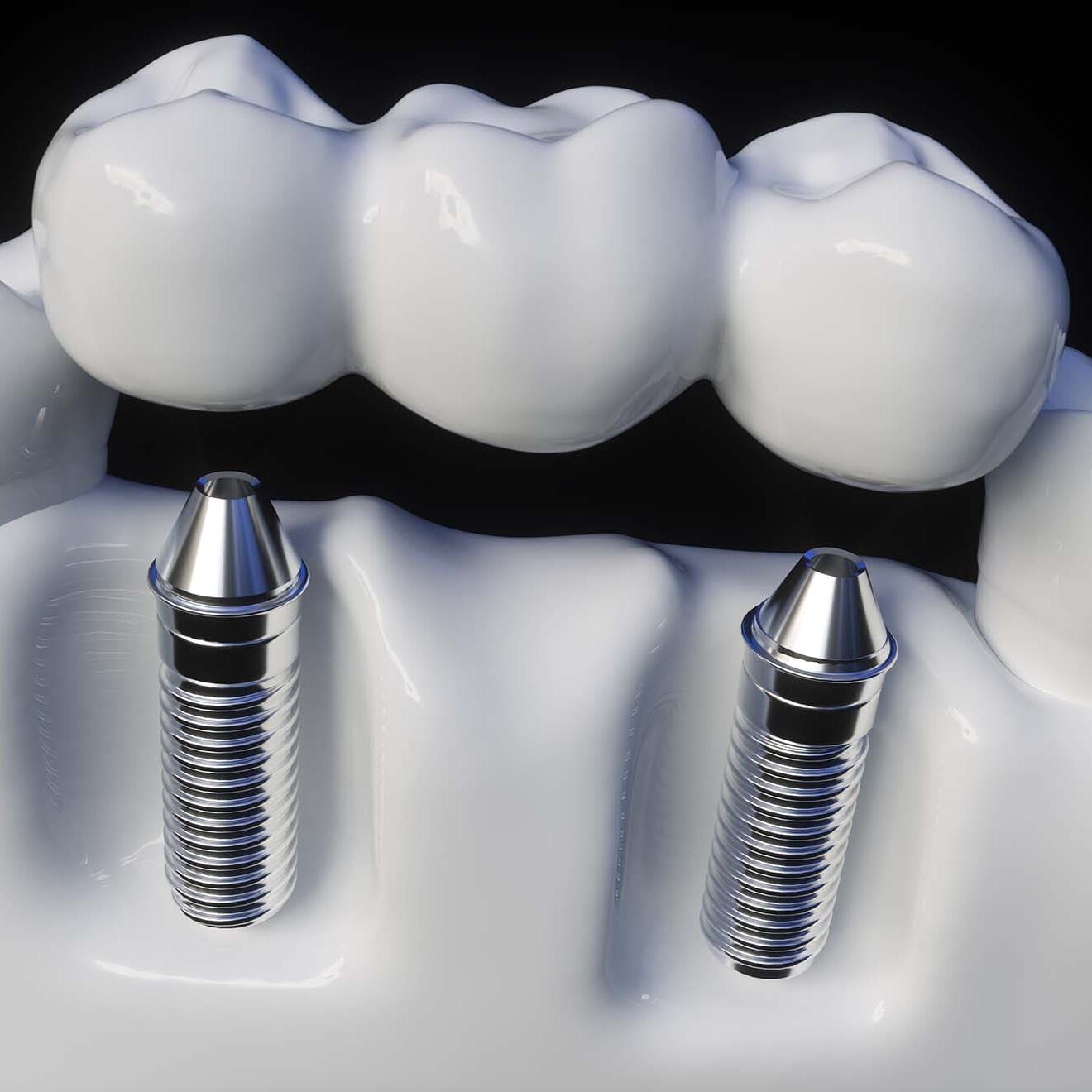
Implant supported overdentures is a type of removable denture connected to dental
implants. The implants are fitted with a special mechanism that clicks with the dentures to
lock them securely. It is different from traditional dentures, which sit directly on the gum
tissues.
Implant-Supported Removable Partial Dentures
Treatment
About This Treatment
The Process
Implant-supported removable partial dentures (RPDs) combine
the benefits of dental implants with the flexibility of partial
dentures. This hybrid solution is especially suitable for patients
who have lost multiple teeth but not all teeth in an arch. The
implants provide stability and prevent bone resorption, while
the removable nature of the denture offers ease of cleaning
and maintenance. Here’s a general overview of the procedure
for placing implant-supported RPDs:
Consultation and Assessment
- Dental Examination:
- Comprehensive oral evaluation, including an assessment of gums, remaining teeth, and bone structure.
- Digital Imaging:
- Obtaining X-rays or CT scans to evaluate the jawbone quality and plan the implant placement.
- Treatment Discussion:
- Discussing the procedure, benefits, potential complications, and alternative treatment options.
Implant Placement
- Anesthesia:
- Administering local anesthesia to numb the surgical area. Sedation might also be provided if necessary.
- Surgical Procedure:
- Drilling holes at pre-determined locations in the jawbone and placing the dental implants. Typically, two or more implants are placed to support the RPD.
Healing and Osseointegration
- Healing Time:
- Allowing several weeks to months for the implants to securely fuse with the jawbone, a process called osseointegration.
- Temporary Prosthesis:
- A temporary partial denture might be provided for aesthetics and function during the healing period.
Design and Fabrication of the Implant-Supported RPD
- Dental Impressions:
- Taking precise impressions or digital scans of the mouth to design the RPD.
- RPD Fabrication:
- Designing the RPD in a dental laboratory, ensuring it incorporates attachments that will connect to the implants.
Fitting and Adjusting the RPD
- Initial Fit:
- Trying in the RPD to ensure a comfortable fit, optimal bite, and satisfactory aesthetics.
- Adjustments:
- Making any necessary adjustments for comfort and function.
- Educating on Attachments:
- Instructing the patient on how to attach and detach the RPD from the implants.
Post-Placement Care and Follow-Up
- Instruction on Care:
- Providing guidelines on cleaning the RPD, maintaining oral hygiene, and caring for the implants.
- Regular Dental Check-ups:
- Monitoring the health and stability of the implant-supported RPD and the surrounding oral structures through routine dental visits.
- Routine Cleanings:
- Regular professional cleanings to ensure the longevity of the RPD and implants.
- Periodic Adjustments:
- Making any necessary adjustments or repairs to the RPD over time, ensuring ongoing comfort and function.
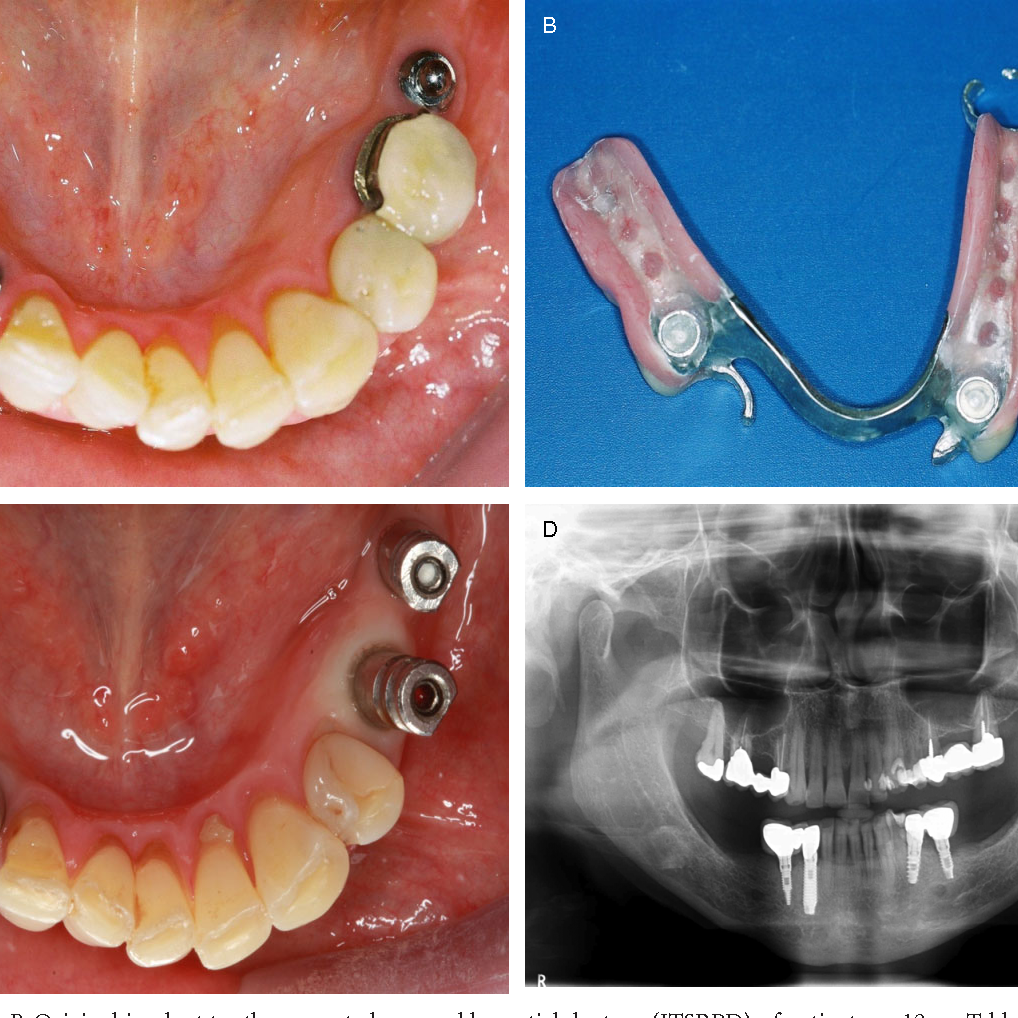
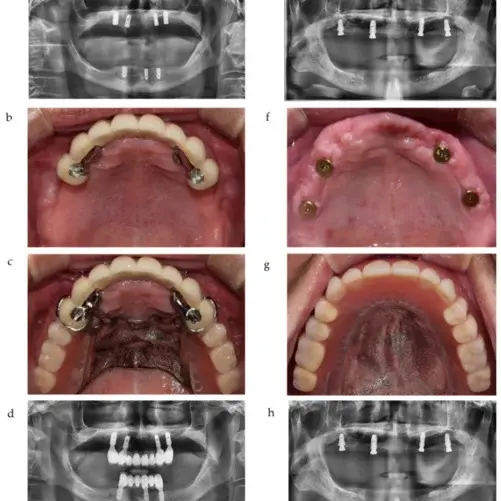
Before and After
SEE OUR RESULTS
Patient Stories
The Dental Implant Institute has been an excellent dentist surgery that I have been attending as a patient for many years. When I was young I didn’t have a pleasant experience with my local dentist on more than one occasion. I found the dentist at The Dental Implant Institute very reassuring and comforting. The management…
A great surgery; Dr Javier in particular spent time with me to make sure my new night guards fitted well and were up to the job
I lost my two front teeth whilst at school and had complications for years. Unfortunately I ended up needing an implant – which I had been avoiding! I wish I had done it sooner. Dr Javier was fantastic and guided me through each stage. He was always contactable to answer any queries or concerns. Very…
FAQs
Can a partial denture be attached to an implant?
If you have only received a few corrective dental implants, and a looking to gain additional, your dental implants can be used as a great foundation for partial denture placements.
Is implant supported denture fixed or removable?
The difference between the two options is that removable implant-supported dentures can be snapped on and off of the abutments whenever you need to remove them, while fixed dentures are permanent and can only be removed by a dentist.
Can you sleep with implant supported dentures?
As with any type of denture, it is necessary to remove implant-supported dentures from the mouth before going to bed at night. There are a few reasons why this is necessary, with one of the more important reasons being that the gum tissues need to rest.
Can you elaborate on the structure and functionality of implant-supported removable partial dentures?
Implant-supported removable partial dentures (ISRPDs) represent a convergence of traditional removable prosthetics and contemporary implantology, orchestrating a symbiotic relationship that leverages the stability of implants while retaining the adaptability of a removable prosthesis. The structure essentially incorporates dental implants, usually integrated into the jawbone, which engage with specific attachments housed within the partial denture. This union not only confers enhanced stability and retention to the denture but also mitigates the classic limitations of conventional removable partial dentures, such as movement during function and potential tissue irritation. The functionality extends to improved masticatory efficiency, enriched aesthetic harmony, and enhanced prosthetic longevity, while still permitting the patient to remove the prosthesis for hygiene and maintenance.
How do ISRPDs enhance the patient’s functional and aesthetic experiences compared to traditional removable partial dentures?
The incorporation of dental implants into the prosthetic solution significantly uplifts the functional and aesthetic paradigms experienced by the patient. From a functional standpoint, ISRPDs diminish the traditional challenges associated with removable prosthetics such as inadvertent movement, potential dislodgement during speech or mastication, and pressure spots. Aesthetically, the enhanced stability enables more natural and harmonious integration of prosthetic teeth, potentially eliminating the need for visible clasps and facilitating more natural-looking transitions between prosthetic and natural dentition. The secure foundation provided by the implants and the precision attachments further allows for a more confident and unrestrained social and functional engagement for the patient.
Can ISRPDs serve as a viable option for patients with significant bone loss?
Indeed, ISRPDs can serve as a particularly viable option for patients encountering significant bone loss, provided certain clinical parameters are met. The strategic placement of implants, possibly combined with minor bone augmentation procedures, facilitates the integration of ISRPDs even amidst a backdrop of compromised bone volume. The implants not only provide a stable foundation for the partial denture but also contribute to mitigating further bone resorption by providing functional stimulation to the residual alveolar bone, which might be notably absent with traditional removable partial dentures.
What does the procedural journey towards acquiring ISRPDs typically involve, and how does it compare to conventional denture processes?
The procedural journey towards ISRPDs encompasses a blend of surgical and prosthetic phases that harmoniously integrate the placement and restoration of dental implants with the fabrication of a removable partial denture. Initial phases involve comprehensive evaluations, radiographic analyses, and treatment planning, which are followed by the surgical placement of dental implants in the jawbone. Following an appropriate healing and osseointegration period, precision attachments are affixed to the implants, and the corresponding removable partial denture is fabricated with complementary receptacles, ensuring a secure yet removable engagement. Contrasting with conventional dentures, the journey involves surgical components and a more intricate prosthetic orchestration to harmonize the implant and removable elements, culminating in a solution that combines the merits of stability and removability.
What maintenance considerations are pertinent for ISRPDs, and how do they influence longevity and functionality?
Maintenance considerations for ISRPDs extend beyond those for traditional removable prosthetics, necessitating a meticulous amalgamation of implant maintenance and removable prosthetic care. Regular and thorough cleaning of both the partial denture and the implant components is paramount, ensuring the mitigation of bacterial accumulation and potential peri-implant concerns. Periodic professional evaluations ensure optimal health of the supporting tissues, the integrity of the prosthetic components, and the functional harmony of the occlusion, thereby influencing longevity and sustained functionality. Wear and tear of the removable elements and attachments may necessitate adjustments or replacements over time to ensure the continued stability and efficacy of the ISRPD.
How does the patient’s quality of life and oral function transition post-adoption of ISRPDs?
Adoption of ISRPDs often precipitates a notable enhancement in the patient’s quality of life and oral function. The substantive stability provided by the implants significantly uplifts masticatory efficiency, enabling the patient to engage in a wider dietary repertoire with confidence. Aesthetically, the secure foundation facilitates a more natural integration of prosthetic elements, enhancing visual harmony and potentially enriching social interactions. Furthermore, the mitigated movement and enhanced retention contribute to improved speech articulation and reduced potential for discomfort, thereby transitioning the patient’s experience towards a more functionally unrestrained and aesthetically harmonious paradigm.
Are there specific clinical scenarios where ISRPDs might be contraindicated, and what alternatives might be explored in such instances?
Certain clinical scenarios, such as uncontrolled systemic conditions that may impede surgical or overall treatment success, compromised oral hygiene, or the inability to comply with requisite maintenance protocols, might contraindicate the adoption of ISRPDs. In instances where ISRPDs are not feasible, alternative treatment avenues such as conventional removable partial dentures, implant-supported fixed partial dentures, or exploring advanced reconstructive options to facilitate fixed implant solutions might be considered, ensuring that the chosen pathway resonates harmoniously with the patient’s clinical, functional, and aesthetic landscapes.
Book your consultation
Every journey begins with a detailed consultation. Our approach is always
bespoke, and your plan is individualised for you and your concerns.