Socket preservation is a surgical procedure whose aim is to limit the physiological resorption
of the alveolar ridge that occurs after a dental extraction, in order to have sufficient bone to
perform an implant placement.
Socket Preservation
Treatment
About This Treatment
The Process
Socket preservation is a vital procedure employed post-tooth
extraction to safeguard and uphold the structure of the socket,
ensuring optimal conditions for future tooth replacement
options like dental implants. Here’s a step-by-step breakdown
of a typical socket preservation procedure:
Comprehensive Evaluation
- Dental Examination:
- Detailed inspection of oral health and determination of the need for extraction and socket preservation.
- Imaging:
- Utilizing X-rays or CT scans to assess the bone and surrounding structures.
- Discussion:
- Exploring procedure specifics, benefits, and potential future tooth replacement options.
Tooth Extraction
- Anesthesia:
- Administering local anesthesia to numb the area.
- Tooth Removal:
- Extracting the tooth with care to minimize trauma to the surrounding tissues.
- Cleaning:
- Thoroughly cleansing the socket to remove any residual debris or infection.
Socket Preservation Procedure
- Bone Grafting Material:
- Placing graft material, which can be of various types, into the socket to support bone growth.
- Membrane Application:
- Optionally, covering the graft with a biocompatible membrane to foster optimal healing and to prevent soft tissue from entering the graft site.
- Suturing:
- Closing the gum tissue with sutures to secure the graft and membrane.
Recovery Period
- Post-Operative Care:
- Following detailed guidelines regarding oral hygiene, diet, and physical activity to promote smooth recovery.
- Healing Time:
- Allowing several months for the bone graft to integrate and for the site to heal adequately.
Future Dental Restoration Planning
- Assessment:
- Evaluating the success of the socket preservation and determining adequate bone volume and quality for subsequent restoration.
- Implant Placement (if applicable):
- Once sufficient healing has occurred, planning for dental implant placement or another suitable tooth replacement option.
- Restoration:
- Finalizing the restoration process with a dental crown, bridge, or denture as per the pre-decided plan.
Ongoing Monitoring and Care
- Regular Dental Check-ups:
- Ensuring routine dental visits for professional cleanings and to keep an eye on the health and stability of the restoration and adjacent structures.
- Maintain Oral Hygiene:
- Practicing diligent oral care to uphold the health and longevity of the restoration.
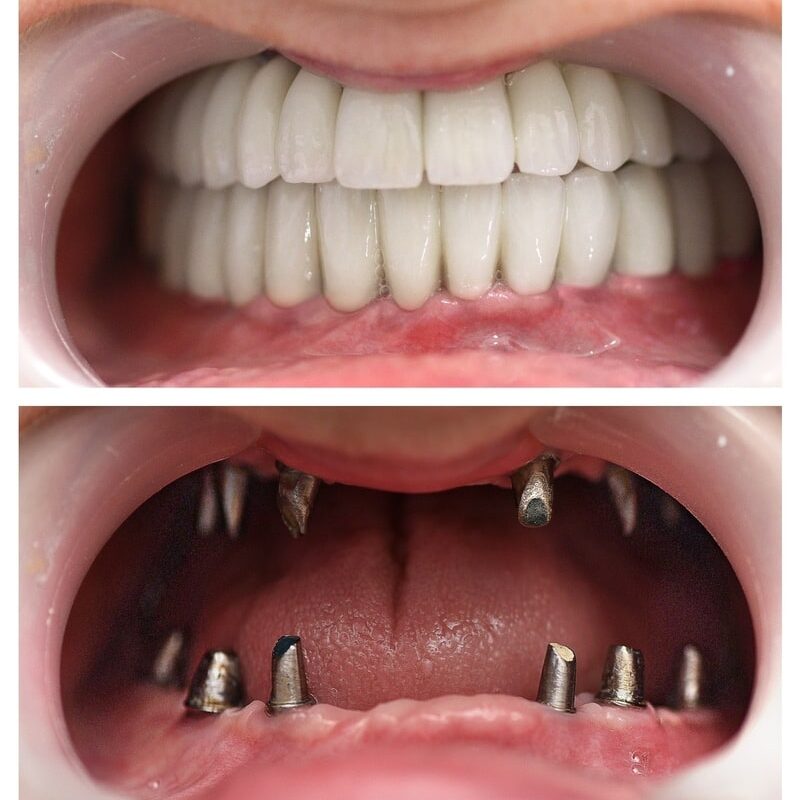
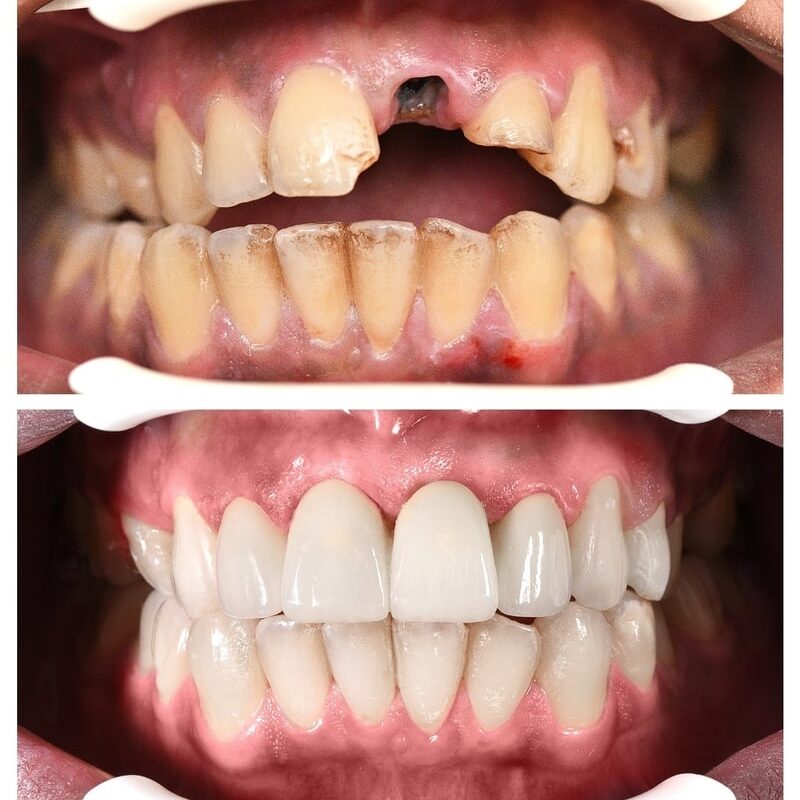
Before and After
SEE OUR RESULTS
Patient Stories
The Dental Implant Institute has been an excellent dentist surgery that I have been attending as a patient for many years. When I was young I didn’t have a pleasant experience with my local dentist on more than one occasion. I found the dentist at The Dental Implant Institute very reassuring and comforting. The management…
A great surgery; Dr Javier in particular spent time with me to make sure my new night guards fitted well and were up to the job
I lost my two front teeth whilst at school and had complications for years. Unfortunately I ended up needing an implant – which I had been avoiding! I wish I had done it sooner. Dr Javier was fantastic and guided me through each stage. He was always contactable to answer any queries or concerns. Very…
FAQs
What is socket preservation technique?
Socket preservation or alveolar ridge preservation is a procedure to reduce bone loss after tooth extraction. After tooth extraction, the jaw bone has a natural tendency to become narrow, and lose its original shape because the bone quickly resorbs, resulting in 30–60% loss in bone volume in the first six months.
How long does socket preservation graft last?
Generally, a bone graft permanently fuses with your natural jawbone. It can last forever. However, if an implant doesn’t replace a tooth, the new bone density will deteriorate gradually due to a lack of chewing stimulation. You can expect significant jawbone loss within the first 12 months.
Can socket preservation impact the timeline and outcome of future implant placement?
Absolutely, socket preservation exercises a pivotal influence on both the chronological and clinical trajectory of subsequent implant placement. By curtailing the propensity for alveolar bone resorption post-extraction and maintaining the spatial and structural integrity of the socket, this practice fosters a robust foundation for implant integration. Additionally, it minimizes the potential need for more invasive and extensive bone grafting procedures at the time of implant placement, thereby potentially abbreviating and simplifying the implantological journey, and ensuring aesthetically and functionally harmonious outcomes.
What materials are typically employed during a socket preservation procedure?
Socket preservation embraces a diverse palette of materials, each chosen based on the clinical scenario, practitioner preference, and patient-specific factors. The bone graft material, which can be autogenous, allogenic, xenogenic, or alloplastic, forms the structural cornerstone of the procedure. Further, membranes, which can be resorbable or non-resorbable, are utilized to shield the graft, facilitating optimal osteogenesis and preventing ingrowth of undesirable soft tissue. Suturing materials, which may be absorbable or non-absorbable, secure the soft tissue, ensuring a stable and protective environment for the regenerative process.
Who is an ideal candidate for socket preservation, and are there situations where it might not be recommended?
While socket preservation is frequently advocated following extractions to safeguard structural integrity, ideal candidacy is nuanced by factors such as the patient’s overall health, the condition of adjacent structures, and future prosthetic plans. Generally, individuals poised for future implant placement or those keen on preserving aesthetic and structural harmony are ideal candidates. Scenarios where it might be judiciously omitted or modified include instances of acute infection, compromised systemic health, or cases where alternative treatment pathways are delineated based on comprehensive clinical evaluation.
What does the post-procedure care and recovery entail after socket preservation?
Post-procedure care following socket preservation involves a meticulous confluence of protecting the surgical site, adhering to prescribed pharmacologic management, and ensuring optimal oral hygiene without disturbing the regenerative process. Patients are guided to avoid undue pressure or trauma to the site, adhere to a conducive dietary regimen, and follow a tailored oral hygiene protocol that circumvents disruption of the healing site while maintaining overall oral health. Regular follow-up appointments ensure the trajectory of healing and recovery is monitored, optimizing outcomes, and navigating any potential post-operative concerns.
Is socket preservation a universally standardized procedure, or are there variations in its execution?
While the fundamental ethos of socket preservation—being the conservation of alveolar bone post-extraction—is universally acknowledged, variations in technique, material selection, and ancillary procedures may be sculpted based on clinical presentation, practitioner preference, and evolving scientific evidence. Different clinicians might leverage diverse graft materials, membranes, or employ adjunctive procedures such as PRF (Platelet-Rich Fibrin) based on the individualized needs of the patient and the clinical scenario, thus tailoring the procedure to optimize regenerative outcomes in a personalized manner.
What potential complications should be considered in socket preservation procedures?
Complications, while relatively rare when socket preservation is executed meticulously, can encompass aspects such as infection, graft or membrane displacement, prolonged healing, or suboptimal bone regeneration. Precise surgical technique, rigorous post-operative management, and adherence to post-care instructions significantly mitigate these risks, ensuring that the regenerative process unfolds in a clinically optimal manner, thereby paving the way for successful future prosthetic endeavors.
London Coverage
We provide dental treatments to patients across the whole of London and have provided specialist dental Implant treatments to patients in areas such as: Aldgate, Bow, Barnet, Camden, Chelsea, Clapham, Clapton, Croydon, Dalston, Deptford, Dulwich, Ealing, Fulham, Hackney, Hammersmith, Hanwell, Hendon, Highbury, Highgate, Isle of Dogs, Islington, Mile End, Millwall, New Cross, Plaistow, Poplar, Shoreditch, Stepney, Streatham, Sutton, Totteridge, Tower Hill, Twickenham, Watford, Whetstone, White Chapel and Wimbledon.
Book your consultation
Every journey begins with a detailed consultation. Our approach is always
bespoke, and your plan is individualised for you and your concerns.