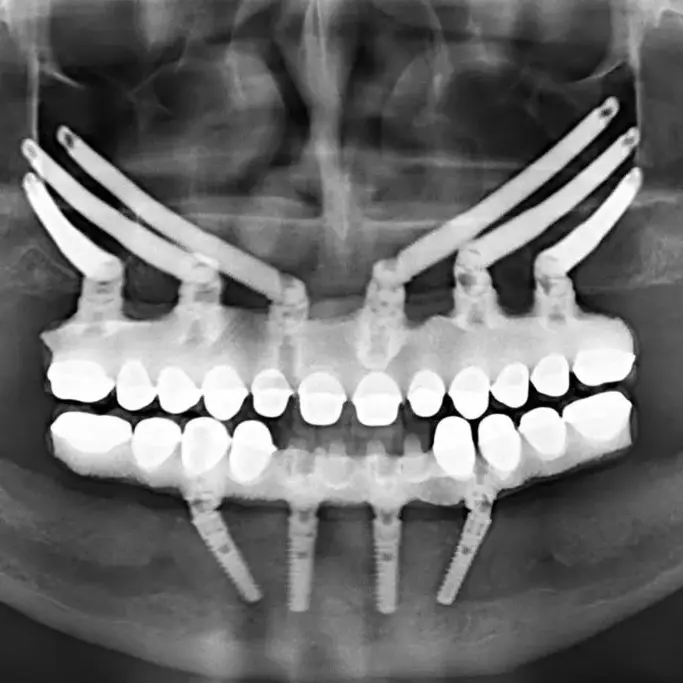
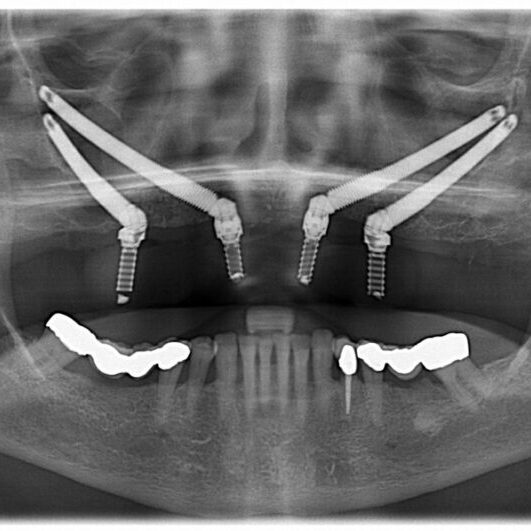
Zygomatic implants are intended to replace teeth in the upper jaw. They can be used to
replace an entire arch of missing teeth, severely damaged or decayed teeth, or teeth that
have become loose due to severe periodontal disease.
Zygomatic Implants
Treatment
About This Treatment
The Process
Zygomatic implants offer a dental rehabilitation solution for
patients with significant maxillary (upper jaw) bone loss. Unlike
conventional dental implants, zygomatic implants are anchored
in the zygomatic bone (cheekbone), providing an alternative for
patients who might otherwise require extensive bone grafting.
Here’s an overview of the procedure:
Consultation and Assessment
- Oral Examination:
- Detailed analysis of oral health and existing bone structure.
- Imaging Studies:
- Employing CT scans to evaluate the zygomatic bone and plan the implant placement meticulously.
- Treatment Discussion:
- Outlining the procedure, risks, benefits, alternatives, and addressing patient queries.
Pre-Procedural Steps
- Health Evaluation:
- Reviewing medical history and managing any existing health conditions.
- Preparation of Prosthesis:
- Pre-fabrication of the prosthesis may be done to potentially enable immediate loading post-surgery.
Healing and Osseointegration
- Recovery Protocols:
- Adhering to specific post-operative care instructions, including diet, oral hygiene practices, and activity restrictions.
- Follow-Up Appointments:
- Monitoring the healing process and ensuring the stability and integration of the implants through scheduled visits.
Fabrication of the Final Prosthesis
- Assessment of Integration:
- Confirming osseointegration of the zygomatic implants through clinical evaluation and possibly additional imaging.
- Final Restoration:
- Attaching the final prosthesis, which could be a fixed bridge or overdenture, ensuring optimal function and aesthetics.
Follow-Up and Maintenance
- Oral Hygiene:
- Upholding meticulous oral care to maintain the health of the implants and surrounding tissues.
- Routine Check-Ups:
- Engaging in regular dental visits for professional cleanings and to monitor the stability and health of the zygomatic implants and prosthesis.
Long-Term Success
- Proactive Management:
- Addressing any issues promptly to safeguard the longevity of the zygomatic implants and overall oral health.
- Periodic Reviews:
- Undergoing periodic assessments to ensure the continued functionality and aesthetics of the implant-supported prosthesis.
Before and After
SEE OUR RESULTS
Patient Stories
The Dental Implant Institute has been an excellent dentist surgery that I have been attending as a patient for many years. When I was young I didn’t have a pleasant experience with my local dentist on more than one occasion. I found the dentist at The Dental Implant Institute very reassuring and comforting. The management…
A great surgery; Dr Javier in particular spent time with me to make sure my new night guards fitted well and were up to the job
I lost my two front teeth whilst at school and had complications for years. Unfortunately I ended up needing an implant – which I had been avoiding! I wish I had done it sooner. Dr Javier was fantastic and guided me through each stage. He was always contactable to answer any queries or concerns. Very…
FAQs
What if I don’t have enough bone for dental implants?
The CBCT scan lets us know in advance of dental implant treatment if you don’t have the necessary height and width of bone. In this case, we can augment the bone using a bone graft, which can be done before or at the same time as your cosmetic teeth implant surgery.
What are the disadvantages of zygomatic implants?
Though rare, additional issues that have the potential to develop during or following Zygomatic implant surgery include:
- Vestibular cortical fenestration.
- Temporary sensory nerve deficits.
- Orbital penetration and injury.
- Oroantral fistula formation.
- Subconjunctival and periorbital.
- Intraoral soft tissue problems.
How long do zygomatic implants last?
Zygomatic dental implants are made of high-quality materials, and, with proper care, they can last a lifetime. However, just like traditional dental implants, the lifespan of a zygomatic implant can vary from patient to patient, depending on factors such as oral hygiene and overall health.
Are zygomatic implants safe?
Yes, even though the implants are attached to your zygomatic bone, (which does sound painful) the process actually causes less trauma than using a bone graft. The application process is done through intravenous sedation, so you won’t feel a thing.
Can you elucidate what zygomatic implants are and their primary utilization in dental implantology?
Zygomatic implants stand as specialized dental implants, meticulously designed to engage the zygoma, or cheekbone, providing a robust and stable anchorage in scenarios characterized by significant maxillary (upper jaw) bone deficiency. Their deployment primarily caters to patients presenting with substantive maxillary atrophy, offering a viable, often less invasive alternative to traditional bone grafting procedures. Zygomatic implants traverse through or alongside the maxillary sinus, anchoring into the dense zygomatic bone, thus facilitating prosthetic rehabilitation in areas where conventional implants might be clinically unfeasible due to insufficient bone substrate.
What does the procedural deployment of zygomatic implants encompass, and how does it differentiate from conventional implant placement?
The procedural execution of zygomatic implants encompasses a tailored surgical approach, which extends beyond the traditional horizons of implant placement. Given the distinct anatomy of the zygomatic region and the specific trajectory of these implants, the surgical protocol necessitates adept knowledge and navigation of the maxillofacial structures. Unlike conventional implants which are anchored into the alveolar bone, zygomatic implants traverse through the maxilla, potentially bypassing the maxillary sinus, to secure into the zygomatic bone, thereby providing a stable foundation amidst a backdrop of maxillary bone deficiency.
What are the key indications that position zygomatic implants as a preferential choice over other dental implant solutions?
Key indications steering the preference towards zygomatic implants often revolve around substantial maxillary bone loss, which might render traditional implant placement unfeasible without extensive bone grafting. Patients who have experienced significant resorption of the upper jaw, those with maxillary defects or have undergone maxillectomy, and situations where sinus anatomy or health precludes sinus lifting or grafting, might emerge as quintessential candidates for zygomatic implants. Furthermore, individuals seeking to circumvent more extensive grafting procedures might find a harmonious solution in zygomatic implants.
Is the aesthetic outcome influenced or compromised due to the specialized trajectory of zygomatic implants?
Aesthetic outcomes with zygomatic implants, when harmoniously orchestrated through meticulous planning and prosthetic execution, can parallel, if not surpass, those achieved with conventional implant protocols. The strategic positioning and trajectory of zygomatic implants, while primarily functional in intention, are also designed to support prosthetic solutions that align seamlessly with the aesthetic expectations and facial harmony of the patient, thereby ensuring that the restorative outcome resonates both functionally and aesthetically with the patient’s needs.
Are there any specific post-surgical considerations or care instructions pertinent to zygomatic implants?
Post-surgical care following zygomatic implant placement intertwines general principles of post-implantology care with specific nuances pertinent to the zygomatic anatomy. Vigilance towards avoiding undue pressure or trauma, adherence to prescribed pharmacological management, and maintaining scrupulous oral hygiene, all while ensuring protection of the surgical site, form the core tenets of post-surgical care. Given the proximity to sinus and facial structures, specific instructions pertaining to nasal hygiene, activities influencing sinus pressure, and monitoring of any sinus-related symptoms might be emphasized to ensure a seamless healing journey.
How does the long-term success rate of zygomatic implants compare to that of traditional dental implants?
Zygomatic implants, when deployed judiciously and with adept surgical and prosthetic finesse, have showcased commendable long-term success rates, often paralleling those observed with traditional dental implants. The inherent stability afforded by the dense zygomatic bone, combined with the strategic trajectory and length of the implants, confers a robust foundation for prosthetic rehabilitation. Adherence to rigorous maintenance protocols and regular professional evaluations further fortify the longevity and success of zygomatic implants amidst the unique anatomical and functional landscapes they navigate.
How is patient comfort and experience managed during the surgical placement of zygomatic implants?
Patient comfort and experience during zygomatic implant placement are curated through a meticulous amalgam of anesthesia or sedation, transparent communication, and gentle surgical technique. The choice between local anesthesia, conscious sedation, or general anesthesia is sculpted based on the complexity of the procedure, patient preference, and medical history, ensuring a comfortable and serene procedural journey. Continuous dialogue regarding what to expect during and post-procedure, coupled with empathetic and patient-centric care, further embellishes the patient experience, transforming it into a comfortable and predictably positive endeavor.
London Coverage
We provide dental treatments to patients across the whole of London and have provided specialist dental Implant treatments to patients in areas such as: Aldgate, Bow, Barnet, Camden, Chelsea, Clapham, Clapton, Croydon, Dalston, Deptford, Dulwich, Ealing, Fulham, Hackney, Hammersmith, Hanwell, Hendon, Highbury, Highgate, Isle of Dogs, Islington, Mile End, Millwall, New Cross, Plaistow, Poplar, Shoreditch, Stepney, Streatham, Sutton, Totteridge, Tower Hill, Twickenham, Watford, Whetstone, White Chapel and Wimbledon.
Book your consultation
Every journey begins with a detailed consultation. Our approach is always
bespoke, and your plan is individualised for you and your concerns.